Search
- Page Path
- HOME > Search
- Diabetes, obesity and metabolism
- Triglyceride-Glucose Index Predicts Future Atherosclerotic Cardiovascular Diseases: A 16-Year Follow-up in a Prospective, Community-Dwelling Cohort Study
- Joon Ho Moon, Yongkang Kim, Tae Jung Oh, Jae Hoon Moon, Soo Heon Kwak, Kyong Soo Park, Hak Chul Jang, Sung Hee Choi, Nam H. Cho
- Endocrinol Metab. 2023;38(4):406-417. Published online August 3, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1703

- 2,690 View
- 166 Download
- 3 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
While the triglyceride-glucose (TyG) index is a measure of insulin resistance, its association with cardiovascular disease (CVD) has not been well elucidated. We evaluated the TyG index for prediction of CVDs in a prospective large communitybased cohort.
Methods
Individuals 40 to 70 years old were prospectively followed for a median 15.6 years. The TyG index was calculated as the Ln [fasting triglycerides (mg/dL)×fasting glucose (mg/dL)/2]. CVDs included any acute myocardial infarction, coronary artery disease or cerebrovascular disease. We used a Cox proportional hazards model to estimate CVD risks according to quartiles of the TyG index and plotted the receiver operating characteristics curve for the incident CVD.
Results
Among 8,511 subjects (age 51.9±8.8 years; 47.5% males), 931 (10.9%) had incident CVDs during the follow-up. After adjustment for age, sex, body mass index, diabetes mellitus, hypertension, total cholesterol, smoking, alcohol, exercise, and C-reactive protein, subjects in the highest TyG quartile had 36% increased risk of incident CVD compared with the lowest TyG quartile (hazard ratio, 1.36; 95% confidence interval, 1.10 to 1.68). Carotid plaque, assessed by ultrasonography was more frequent in subjects in the higher quartile of TyG index (P for trend=0.049 in men and P for trend <0.001 in women). The TyG index had a higher predictive power for CVDs than the homeostasis model assessment of insulin resistance (HOMA-IR) (area under the curve, 0.578 for TyG and 0.543 for HOMA-IR). Adding TyG index on diabetes or hypertension alone gave sounder predictability for CVDs.
Conclusion
The TyG index is independently associated with future CVDs in 16 years of follow-up in large, prospective Korean cohort. -
Citations
Citations to this article as recorded by- Construction and validation of a nomogram for predicting diabetes remission at 3 months after bariatric surgery in patients with obesity combined with type 2 diabetes mellitus
Kaisheng Yuan, Bing Wu, Ruiqi Zeng, Fuqing Zhou, Ruixiang Hu, Cunchuan Wang
Diabetes, Obesity and Metabolism.2024; 26(1): 169. CrossRef - Association between the triglyceride glucose index and chronic total coronary occlusion: A cross-sectional study from southwest China
Kaiyong Xiao, Huili Cao, Bin Yang, Zhe Xv, Lian Xiao, Jianping Wang, Shuiqing Ni, Hui Feng, Zhongwei He, Lei Xv, Juan Li, Dongmei Xv
Nutrition, Metabolism and Cardiovascular Diseases.2024; 34(4): 850. CrossRef - The association between TyG and all-cause/non-cardiovascular mortality in general patients with type 2 diabetes mellitus is modified by age: results from the cohort study of NHANES 1999–2018
Younan Yao, Bo Wang, Tian Geng, Jiyan Chen, Wan Chen, Liwen Li
Cardiovascular Diabetology.2024;[Epub] CrossRef - Triglyceride-glucose index predicts type 2 diabetes mellitus more effectively than oral glucose tolerance test-derived insulin sensitivity and secretion markers
Min Jin Lee, Ji Hyun Bae, Ah Reum Khang, Dongwon Yi, Mi Sook Yun, Yang Ho Kang
Diabetes Research and Clinical Practice.2024; 210: 111640. CrossRef - Evaluation of the novel three lipid indices for predicting five- and ten-year incidence of cardiovascular disease: findings from Kerman coronary artery disease risk factors study (KERCADRS)
Alireza Jafari, Hamid Najafipour, Mitra Shadkam, Sina Aminizadeh
Lipids in Health and Disease.2023;[Epub] CrossRef
- Construction and validation of a nomogram for predicting diabetes remission at 3 months after bariatric surgery in patients with obesity combined with type 2 diabetes mellitus

- Clinical Study
- Identification of Novel Genetic Variants Related to Trabecular Bone Score in Community-Dwelling Older Adults
- Sung Hye Kong, Ji Won Yoon, Jung Hee Kim, JooYong Park, Jiyeob Choi, Ji Hyun Lee, A Ram Hong, Nam H. Cho, Chan Soo Shin
- Endocrinol Metab. 2020;35(4):801-810. Published online November 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.735
- 4,622 View
- 112 Download
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
As the genetic variants of trabecular bone microarchitecture are not well-understood, we performed a genome-wide association study to identify genetic determinants of bone microarchitecture analyzed by trabecular bone score (TBS).
Methods
TBS-associated genes were discovered in the Ansung cohort (discovery cohort), a community-based rural cohort in Korea, and then validated in the Gene-Environment Interaction and Phenotype (GENIE) cohort (validation cohort), consisting of subjects who underwent health check-up programs. In the discovery cohort, 2,451 participants were investigated for 1.42 million genotyped and imputed markers.
Results
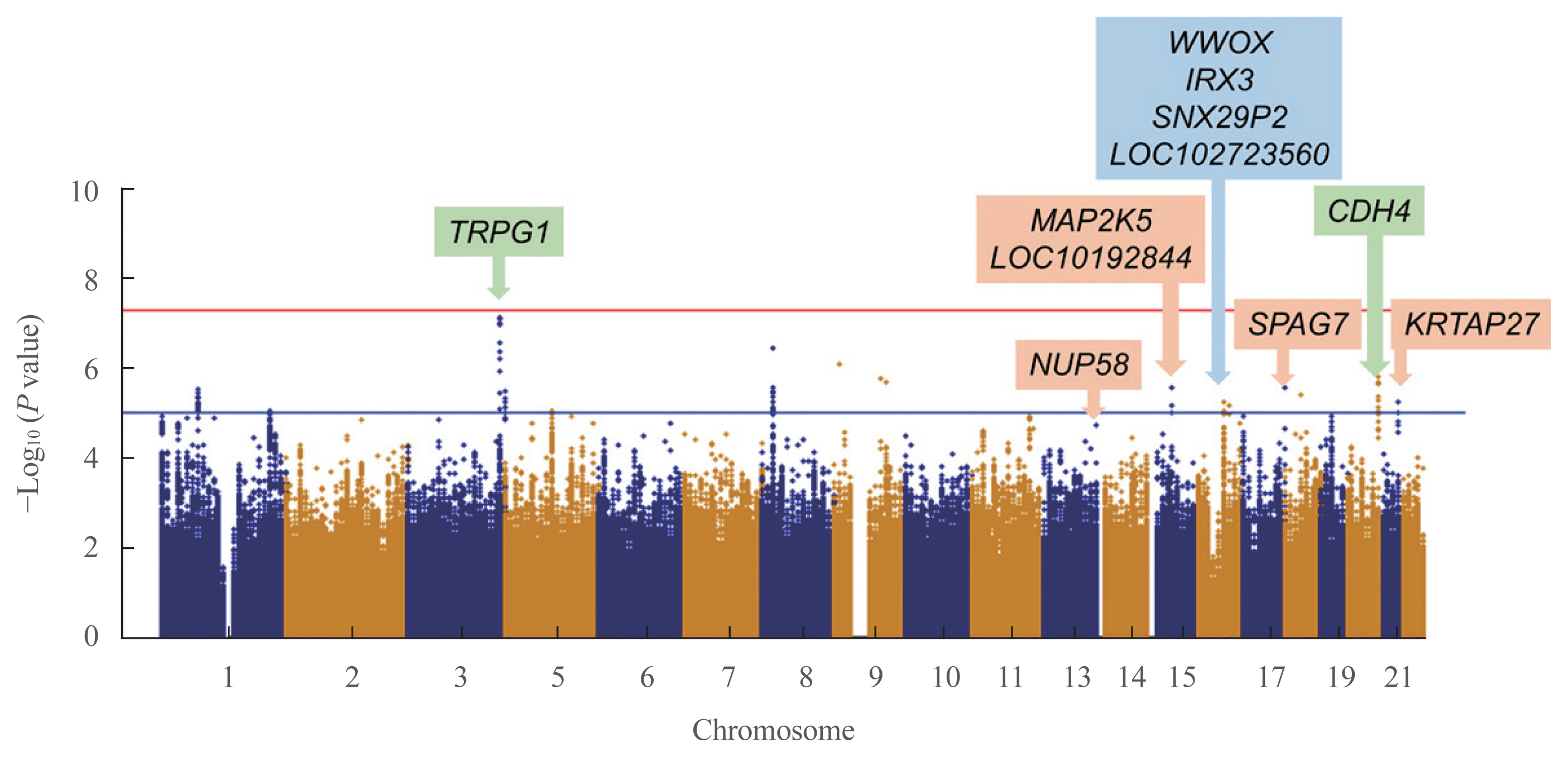
In the validation cohort, identified as significant variants were evaluated in 2,733 participants. An intronic variant in iroquois homeobox 3 (IRX3), rs1815994, was significantly associated with TBS in men (P=3.74E-05 in the discovery cohort, P=0.027 in the validation cohort). Another intronic variant in mitogen-activated protein kinase kinase 5 (MAP2K5), rs11630730, was significantly associated with TBS in women (P=3.05E-09 in the discovery cohort, P=0.041 in the validation cohort). Men with the rs1815994 variant and women with the rs11630730 variant had lower TBS and lumbar spine bone mineral density. The detrimental effects of the rs1815994 variant in men and rs11630730 variant in women were also identified in association analysis (β=–0.0281, β=–0.0465, respectively).
Conclusion
In this study, the rs1815994 near IRX3 in men and rs11630730 near MAP2K5 in women were associated with deterioration of the bone microarchitecture. It is the first study to determine the association of genetic variants with TBS. Further studies are needed to confirm our findings and identify additional variants contributing to the trabecular bone microarchitecture.

- Clinical Study
- Association of Body Mass Index with the Risk of Incident Type 2 Diabetes, Cardiovascular Disease, and All-Cause Mortality: A Community-Based Prospective Study
- Ji Cheol Bae, Nam H. Cho, Jae Hyeon Kim, Kyu Yeon Hur, Sang-Man Jin, Moon-Kyu Lee
- Endocrinol Metab. 2020;35(2):416-424. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.416

- 8,119 View
- 156 Download
- 13 Web of Science
- 12 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Type 2 diabetes and cardiovascular disease (CVD) are the most important sequelae of obesity and the leading cause of death. We evaluated the association between body mass index (BMI) and the risk of incident type 2 diabetes, CVD, and all-cause mortality in a prospective study of a Korean population.
Methods
The shapes of the associations were modeled by restricted cubic splines regression analysis. After categorizing all subjects (n=8,900) into octiles based on their BMI levels, we estimated the hazard ratio (HR) for the association of categorized BMI levels with the risk of incident CVD and type 2 diabetes using a Cox’s proportional hazard analysis.
Results
The mean age of participants was 52 years and 48% were men. Of the subjects at baseline, 39.0% of men and 45.6% of women were classified as obese (BMI ≥25 kg/m2). Over a mean follow-up of 8.1 years, CVD events occurred in 509 participants; 436 died; and 1,258 subjects developed type 2 diabetes. The increased risk of incident diabetes began to be significant at BMI 23 to 24 kg/m2 in both sexes (HR, 1.8). For CVD events, the risk began to increase significantly at BMI 26 to 28 kg/m2 (HR, 1.6). We found a reverse J-shaped relationship between BMI and all-cause mortality, with an increased risk among individuals with BMI values in lower range (BMI <21 kg/m2).
Conclusion
These results suggest that the BMI cut-off points for observed risk were varied depending on the diseases and that the BMI classification of obesity need to be revised to reflect differential risk of obesity-related diseases. -
Citations
Citations to this article as recorded by- Association of obesity with cardiovascular disease in the absence of traditional risk factors
Hui Luo, Yesong Liu, Xue Tian, Yuhan Zhao, Lulu Liu, Zemeng Zhao, Lili Luo, Yanmin Zhang, Xiaozhong Jiang, Yeqiang Liu, Yanxia Luo, Anxin Wang
International Journal of Obesity.2024; 48(2): 263. CrossRef - Clinical characteristics and degree of cardiovascular risk factor control in patients with newly-diagnosed type 2 diabetes in Catalonia
Anna Ramírez-Morros, Josep Franch-Nadal, Jordi Real, Queralt Miró-Catalina, Magdalena Bundó, Bogdan Vlacho, Didac Mauricio
Frontiers in Endocrinology.2024;[Epub] CrossRef - Metabolic status indicators and influencing factors in non-obese, non-centrally obese nonalcoholic fatty liver disease
Zhipeng Huang, Donghong Wei, Xueping Yu, Zicheng Huang, Yijie Lin, Wenji Lin, Zhijun Su, Jianjia Jiang
Medicine.2023; 102(6): e32922. CrossRef - Establishment and health management application of a prediction model for high-risk complication combination of type 2 diabetes mellitus based on data mining
Xin Luo, Jijia Sun, Hong Pan, Dian Zhou, Ping Huang, Jingjing Tang, Rong Shi, Hong Ye, Ying Zhao, An Zhang, Yee Gary Ang
PLOS ONE.2023; 18(8): e0289749. CrossRef - Differential Impact of Obesity on the Risk of Diabetes Development in Two Age Groups: Analysis from the National Health Screening Program
Tae Kyung Yoo, Kyung-Do Han, Yang-Hyun Kim, Ga Eun Nam, Sang Hyun Park, Eun-Jung Rhee, Won-Young Lee
Diabetes & Metabolism Journal.2023; 47(6): 846. CrossRef - Relationship between advanced lung cancer inflammation index and long-term all-cause, cardiovascular, and cancer mortality among type 2 diabetes mellitus patients: NHANES, 1999–2018
Yaying Chen, Mengqian Guan, Ruiqi Wang, Xuewen Wang
Frontiers in Endocrinology.2023;[Epub] CrossRef - Body mass index at baseline directly predicts new-onset diabetes and to a lesser extent incident cardio-cerebrovascular events, but has a J-shaped relationship to all-cause mortality
Yoon-Jong Bae, Sang-Jun Shin, Hee-Taik Kang
BMC Endocrine Disorders.2022;[Epub] CrossRef - Association of Shift Work with Normal-Weight Obesity in Community-Dwelling Adults
Chul Woo Ahn, Sungjae Shin, Seunghyun Lee, Hye-Sun Park, Namki Hong, Yumie Rhee
Endocrinology and Metabolism.2022; 37(5): 781. CrossRef - The Prognostic Value of Combined Status of Body Mass Index and Psychological Well-Being for the Estimation of All-Cause and CVD Mortality Risk: Results from a Long-Term Cohort Study in Lithuania
Dalia Lukšienė, Abdonas Tamosiunas, Ricardas Radisauskas, Martin Bobak
Medicina.2022; 58(11): 1591. CrossRef - The Relationship between Body Mass Index and Incident Diabetes Mellitus in Chinese Aged Population: A Cohort Study
M. L. Tang, Y. Q. Zhou, A. Q. Song, J. L. Wang, Y. P. Wan, R. Y. Xu, Carol Forsblom
Journal of Diabetes Research.2021; 2021: 1. CrossRef - Correlation between adiponectin level and the degree of fibrosis in patients with non-alcoholic fatty liver disease
Manal Sabry Mohamed, Tarek Mohammed Youssef, Esraa Ebrahim Abdullah, Ahmed Elmetwally Ahmed
Egyptian Liver Journal.2021;[Epub] CrossRef - Obesity Measures as Predictors of Type 2 Diabetes and Cardiovascular Diseases among the Jordanian Population: A Cross-Sectional Study
Hana Alkhalidy, Aliaa Orabi, Khadeejah Alnaser, Islam Al-Shami, Tamara Alzboun, Mohammad D. Obeidat, Dongmin Liu
International Journal of Environmental Research and Public Health.2021; 18(22): 12187. CrossRef
- Association of obesity with cardiovascular disease in the absence of traditional risk factors

- Clinical Study
- Low Predictive Value of FRAX Adjusted by Trabecular Bone Score for Osteoporotic Fractures in Korean Women: A Community-Based Cohort Study
- Hana Kim, Jung Hee Kim, Min Joo Kim, A Ram Hong, HyungJin Choi, EuJeong Ku, Ji Hyun Lee, Chan Soo Shin, Nam H. Cho
- Endocrinol Metab. 2020;35(2):359-366. Published online June 24, 2020
- DOI: https://doi.org/10.3803/EnM.2020.35.2.359
- 5,943 View
- 132 Download
- 9 Web of Science
- 10 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The value of the Fracture Risk Assessment Tool (FRAX) and the trabecular bone score (TBS) for assessing osteoporotic fracture risk has not been fully elucidated in Koreans. We conducted this study to clarify the predictive value of FRAX adjusted by TBS for osteoporotic fractures in Korean women.
Methods
After screening 7,192 eligible subjects from the Ansung cohort, 1,165 women aged 45 to 76 years with available bone mineral density (BMD) and TBS data were enrolled in this study. We assessed their clinical risk factors for osteoporotic fractures and evaluated the predictive value of FRAX with or without BMD and TBS.
Results
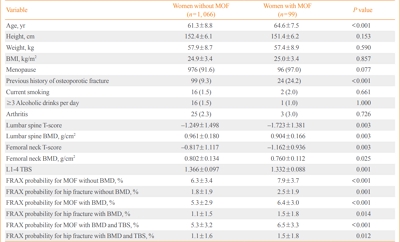
During the mean follow-up period of 7.5 years, 99 (8.5%) women suffered major osteoporotic fractures (MOFs) and 28 (2.4%) experienced hip fractures. FRAX without BMD, BMD-adjusted FRAX, and TBS-adjusted FRAX were significantly associated with the risk of MOFs (hazard ratio [HR] per percent increase, 1.08; 95% confidence interval [CI], 1.03 to 1.14; HR, 1.09; 95% CI, 1.03 to 1.15; and HR, 1.07; 95% CI, 1.02 to 1.13, respectively). However, BMD-adjusted FRAX and TBS-adjusted FRAX did not predict MOFs better than FRAX without BMD based on the Harrell’s C statistic. FRAX probabilities showed limited value for predicting hip fractures. The cut-off values of FRAX without BMD, FRAX with BMD, and FRAX with BMD adjusted by TBS for predicting MOFs were 7.2%, 5.0%, and 6.7%, respectively.
Conclusion
FRAX with BMD and TBS adjustment did not show better predictive value for osteoporotic fractures in this study than FRAX without adjustment. Moreover, the cut-off values of FRAX probabilities for treatment might be lower in Korean women than in other countries. -
Citations
Citations to this article as recorded by- Update on the utility of trabecular bone score (TBS) in clinical practice for the management of osteoporosis: a systematic review by the Egyptian Academy of Bone and Muscle Health
Yasser El Miedany, Walaa Elwakil, Mohammed Hassan Abu-Zaid, Safaa Mahran
Egyptian Rheumatology and Rehabilitation.2024;[Epub] CrossRef - Comparison of predictive value of FRAX, trabecular bone score, and bone mineral density for vertebral fractures in systemic sclerosis: A cross-sectional study
Kyung-Ann Lee, Hyun-Joo Kim, Hyun-Sook Kim
Medicine.2023; 102(2): e32580. CrossRef - Screening for the primary prevention of fragility fractures among adults aged 40 years and older in primary care: systematic reviews of the effects and acceptability of screening and treatment, and the accuracy of risk prediction tools
Michelle Gates, Jennifer Pillay, Megan Nuspl, Aireen Wingert, Ben Vandermeer, Lisa Hartling
Systematic Reviews.2023;[Epub] CrossRef - Chronic airway disease as a major risk factor for fractures in osteopenic women: Nationwide cohort study
Sung Hye Kong, Ae Jeong Jo, Chan Mi Park, Kyun Ik Park, Ji Eun Yun, Jung Hee Kim
Frontiers in Endocrinology.2023;[Epub] CrossRef - Update on the clinical use of trabecular bone score (TBS) in the management of osteoporosis: results of an expert group meeting organized by the European Society for Clinical and Economic Aspects of Osteoporosis, Osteoarthritis and Musculoskeletal Disease
Enisa Shevroja, Jean-Yves Reginster, Olivier Lamy, Nasser Al-Daghri, Manju Chandran, Anne-Laurence Demoux-Baiada, Lynn Kohlmeier, Marie-Paule Lecart, Daniel Messina, Bruno Muzzi Camargos, Juraj Payer, Sansin Tuzun, Nicola Veronese, Cyrus Cooper, Eugene V.
Osteoporosis International.2023; 34(9): 1501. CrossRef - Comparison of HU histogram analysis and BMD for proximal femoral fragility fracture assessment: a retrospective single-center case–control study
Sun-Young Park, Hong Il Ha, Injae Lee, Hyun Kyung Lim
European Radiology.2022; 32(3): 1448. CrossRef - Association of Trabecular Bone Score-Adjusted Fracture Risk Assessment Tool with Coronary Artery Calcification in Women
Tzyy-Ling Chuang, Yuh-Feng Wang, Malcolm Koo, Mei-Hua Chuang
Diagnostics.2022; 12(1): 178. CrossRef - Risk of osteoporotic fracture in women using the FRAX tool with and without bone mineral density score in patients followed at a tertiary outpatient clinic ‒ An observational study
Maria Helena Sampaio Favarato, Maria Flora de Almeida, Arnaldo Lichtenstein, Milton de Arruda Martins, Mario Ferreira Junior
Clinics.2022; 77: 100015. CrossRef - Comparison of Trabecular Bone Score–Adjusted Fracture Risk Assessment (TBS-FRAX) and FRAX Tools for Identification of High Fracture Risk among Taiwanese Adults Aged 50 to 90 Years with or without Prediabetes and Diabetes
Tzyy-Ling Chuang, Mei-Hua Chuang, Yuh-Feng Wang, Malcolm Koo
Medicina.2022; 58(12): 1766. CrossRef - Application of the Trabecular Bone Score in Clinical Practice
Sung Hye Kong, Namki Hong, Jin-Woo Kim, Deog Yoon Kim, Jung Hee Kim
Journal of Bone Metabolism.2021; 28(2): 101. CrossRef
- Update on the utility of trabecular bone score (TBS) in clinical practice for the management of osteoporosis: a systematic review by the Egyptian Academy of Bone and Muscle Health

- Clinical Study
- Glucose-Dependent Insulinotropic Peptide Level Is Associated with the Development of Type 2 Diabetes Mellitus
- Sunghwan Suh, Mi Yeon Kim, Soo Kyoung Kim, Kyu Yeon Hur, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
- Endocrinol Metab. 2016;31(1):134-141. Published online March 16, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.1.134
- 3,821 View
- 44 Download
- 7 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Incretin hormone levels as a predictor of type 2 diabetes mellitus have not been fully investigated. Therefore, we measured incretin hormone levels to examine the relationship between circulating incretin hormones, diabetes, and future diabetes development in this study.
Methods A nested case-control study was conducted in a Korean cohort. The study included the following two groups: the control group (
n =149), the incident diabetes group (n =65). Fasting total glucagon-like peptide-1 (GLP-1) and total glucose-dependent insulinotropic peptide (GIP) levels were measured and compared between these groups.Results Fasting total GIP levels were higher in the incident diabetes group than in the control group (32.64±22.68 pmol/L vs. 25.54±18.37 pmol/L,
P =0.034). There was no statistically significant difference in fasting total GLP-1 levels between groups (1.14±1.43 pmol/L vs. 1.39±2.13 pmol/L,P =0.199). In multivariate analysis, fasting total GIP levels were associated with an increased risk of diabetes (odds ratio, 1.005;P =0.012) independent of other risk factors.Conclusion Fasting total GIP levels may be a risk factor for the development of type 2 diabetes mellitus. This association persisted even after adjusting for other metabolic parameters such as elevated fasting glucose, hemoglobin A1c, and obesity in the pre-diabetic period.
-
Citations
Citations to this article as recorded by- Mendelian randomization analyses suggest a causal role for circulating GIP and IL-1RA levels in homeostatic model assessment-derived measures of β-cell function and insulin sensitivity in Africans without type 2 diabetes
Karlijn A. C. Meeks, Amy R. Bentley, Themistocles L. Assimes, Nora Franceschini, Adebowale A. Adeyemo, Charles N. Rotimi, Ayo P. Doumatey
Genome Medicine.2023;[Epub] CrossRef - Glucose- and Bile Acid-Stimulated Secretion of Gut Hormones in the Isolated Perfused Intestine Is Not Impaired in Diet-Induced Obese Mice
Jenna E. Hunt, Jens J. Holst, Sara L. Jepsen
Frontiers in Endocrinology.2022;[Epub] CrossRef - Combined treatment with a gastric inhibitory polypeptide receptor antagonist and a peptidyl peptidase-4 inhibitor improves metabolic abnormalities in diabetic mice
Fei Yang, Shan Dang, Hongjun LV, Bingyin Shi
Journal of International Medical Research.2021; 49(1): 030006052098566. CrossRef - Elevated levels of fasting serum GIP may be protective factors for diabetic retinopathy in type 2 diabetes mellitus
LingHong Huang, JingXiong Zhou, Bo Liang, HuiBin Huang, LiangYi Li
International Journal of Diabetes in Developing Countries.2021; 41(4): 543. CrossRef - Enteroendocrine K and L cells in healthy and type 2 diabetic individuals
Tina Jorsal, Nicolai A. Rhee, Jens Pedersen, Camilla D. Wahlgren, Brynjulf Mortensen, Sara L. Jepsen, Jacob Jelsing, Louise S. Dalbøge, Peter Vilmann, Hazem Hassan, Jakob W. Hendel, Steen S. Poulsen, Jens J. Holst, Tina Vilsbøll, Filip K. Knop
Diabetologia.2018; 61(2): 284. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef
- Mendelian randomization analyses suggest a causal role for circulating GIP and IL-1RA levels in homeostatic model assessment-derived measures of β-cell function and insulin sensitivity in Africans without type 2 diabetes

- Obesity and Metabolism
- Sex Factors in the Metabolic Syndrome as a Predictor of Cardiovascular Disease
- Sunghwan Suh, Jongha Baek, Ji Cheol Bae, Kyoung-Nyoun Kim, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee
- Endocrinol Metab. 2014;29(4):522-529. Published online December 29, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.4.522
- 4,681 View
- 37 Download
- 16 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background Metabolic syndrome (MetS) is a condition characterized by a cluster of metabolic disorders and is associated with increased risk of cardiovascular disease (CVD). This study analyzed data from the Korean Health and Genome Study to examine the impact of MetS on CVD.
Methods A total of 8,898 subjects (4,241 males and 4,657 females), 40 to 69 years of age, were enrolled and evaluated for the development of new onset CVD from 2001 to 2012 (median 8.1 years of follow-up).
Results The prevalence of MetS at baseline was 22.0% (932/4,241) and 29.7% (1,383/4,657) in males and females, respectively. MetS was associated with increased risk of coronary heart disease (CHD; hazard ratio [HR], 1.818; 95% confidence interval [CI], 1.312 to 2.520 in males; HR, 1.789; 95% CI, 1.332 to 2.404 in females) and CVD (HR, 1.689; 95% CI, 1.295 to 2.204 in males; HR, 1.686; 95% CI, 1.007 to 2.192 in females). Specifically, MetS was associated with risk of future stroke in females only (HR, 1.486; 95% CI, 1.007 to 2.192). Among MetS components, abdominal obesity and hypertension were independent predictors of both CHD and CVD. In addition, a higher number of MetS components correlated with higher CVD risk.
Conclusion MetS is a significant risk factor for the development of CVD although its impact varies between sexes.
-
Citations
Citations to this article as recorded by- Cardiovascular age of workers with different employment categories
Byung-Kook Lee, Jaeouk Ahn, Nam-Soo Kim, Jungsun Park, Yangho Kim
Archives of Environmental & Occupational Health.2022; 77(3): 243. CrossRef - Effects of Anthocyanin-rich Berries on the Risk of Metabolic Syndrome: A Systematic Review and Meta-analysis
Mikkel Roulund Wilken, Max Norman Tandrup Lambert, Christine Bodelund Christensen, Per Bendix Jeppesen
Review of Diabetic Studies.2022; 18(1): 42. CrossRef - Rate and risk factors of metabolic components and component combinations according to hypertension status in Tibetans in a cross-sectional study
Jihong Hu, Brian Thompson, Shuxia Wang, Minhao Guo, Chunjuan Yan, Fengfeng Ding, Peng Guo, Li Chen, Zhuoma Cao, Jianzong Wang
Medicine.2022; 101(43): e31320. CrossRef - Gender differences in changes in metabolic syndrome status and its components and risk of cardiovascular disease: a longitudinal cohort study
Azra Ramezankhani, Fereidoun Azizi, Farzad Hadaegh
Cardiovascular Diabetology.2022;[Epub] CrossRef - The Association of Metabolic Syndrome with the development of cardiovascular disease among Kazakhs in remote rural areas of Xinjiang, China: a cohort study
Wenwen Yang, Shuxia Guo, Haixia Wang, Yu Li, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Yanpeng Song, Changjing Li, Zhuo Ma, Rulin Ma, Jia He
BMC Public Health.2021;[Epub] CrossRef - Serum Arylsulfatase and Acid Phosphatase Activity in Patients with Metabolic Syndrome as a Result of Oxidative Damage to Lysosomes
Dorota M. Olszewska-Słonina
Protein & Peptide Letters.2021; 28(11): 1246. CrossRef - Validation of Risk Prediction Models for Atherosclerotic Cardiovascular Disease in a Prospective Korean Community-Based Cohort
Jae Hyun Bae, Min Kyong Moon, Sohee Oh, Bo Kyung Koo, Nam Han Cho, Moon-Kyu Lee
Diabetes & Metabolism Journal.2020; 44(3): 458. CrossRef - The Prevalence of Obesity and Metabolic Syndrome in the Korean Military Compared with the General Population
Jung Hwan Lee, Da Hea Seo, Min Jung Nam, Geon Hui Lee, Dong Hee Yang, Min Joo Lee, Ung-Rim Choi, Seongbin Hong
Journal of Korean Medical Science.2018;[Epub] CrossRef - Relationship between serum bilirubin levels and cardiovascular disease
Sunghwan Suh, Young Rak Cho, Mi Kyoung Park, Duk Kyu Kim, Nam H. Cho, Moon-Kyu Lee, Christian Herder
PLOS ONE.2018; 13(2): e0193041. CrossRef - Comparison Between Metabolic Syndrome and the Framingham Risk Score as Predictors of Cardiovascular Diseases Among Kazakhs in Xinjiang
Wenwen Yang, Rulin Ma, Xianghui Zhang, Heng Guo, Jia He, Lei Mao, Lati Mu, Yunhua Hu, Yizhong Yan, Jiaming Liu, Jiaolong Ma, Shugang Li, Yusong Ding, Mei Zhang, Jingyu Zhang, Shuxia Guo
Scientific Reports.2018;[Epub] CrossRef - Impact of interactions among metabolic syndrome components on the development of cardiovascular disease among Kazakhs in Xinjiang
Wenwen Yang, Xiang Gao, Xianghui Zhang, Yunhua Hu, Heng Guo, Kui Wang, Yizhong Yan, Jia He, Jingyu Zhang, Jiaolong Ma, Lei Mao, Lati Mu, Jiaming Liu, Shugang Li, Yusong Ding, Mei Zhang, Rulin Ma, Shuxia Guo, Mahesh Narayan
PLOS ONE.2018; 13(10): e0205703. CrossRef - Prediction of cardiovascular disease in Korean population: based on health risk appraisal of national health screening program
Jae Moon Yun, Tae Gon Yoo, Seung-Won Oh, Be Long Cho, Eunyoung Kim, Insob Hwang
Journal of the Korean Medical Association.2017; 60(9): 746. CrossRef - Metabolic Syndrome Is a Strong Risk Factor for Minor Ischemic Stroke and Subsequent Vascular Events
Guang-Sheng Wang, Dao-Ming Tong, Xiao-Dong Chen, Tong-Hui Yang, Ye-Ting Zhou, Xiao-Bo Ma, Gianpaolo Reboldi
PLOS ONE.2016; 11(8): e0156243. CrossRef - Metabolic syndrome related to cardiovascular events in a 10-year prospective study
Laura Kazlauskienė, Jūratė Butnorienė, Antanas Norkus
Diabetology & Metabolic Syndrome.2015;[Epub] CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Impact of Cadmium Exposure on the Association between Lipopolysaccharide and Metabolic Syndrome
Seung Han, Kyoung Ha, Ja Jeon, Hae Kim, Kwan Lee, Dae Kim
International Journal of Environmental Research and Public Health.2015; 12(9): 11396. CrossRef - Heat Killed Lactobacillus reuteri GMNL-263 Reduces Fibrosis Effects on the Liver and Heart in High Fat Diet-Hamsters via TGF-β Suppression
Wei-Jen Ting, Wei-Wen Kuo, Dennis Hsieh, Yu-Lan Yeh, Cecilia-Hsuan Day, Ya-Hui Chen, Ray-Jade Chen, Viswanadha Padma, Yi-Hsing Chen, Chih-Yang Huang
International Journal of Molecular Sciences.2015; 16(10): 25881. CrossRef
- Cardiovascular age of workers with different employment categories


 KES
KES

 First
First Prev
Prev



